|
doi: 10.1016/j.jclinane.2010.08.Hint: No, residual volume and dead space volume are not synonymous. Comparison of volume-controlled and pressure-controlled ventilation in steep Trendelenburg position for robot-assisted laparoscopic radical prostatectomy. 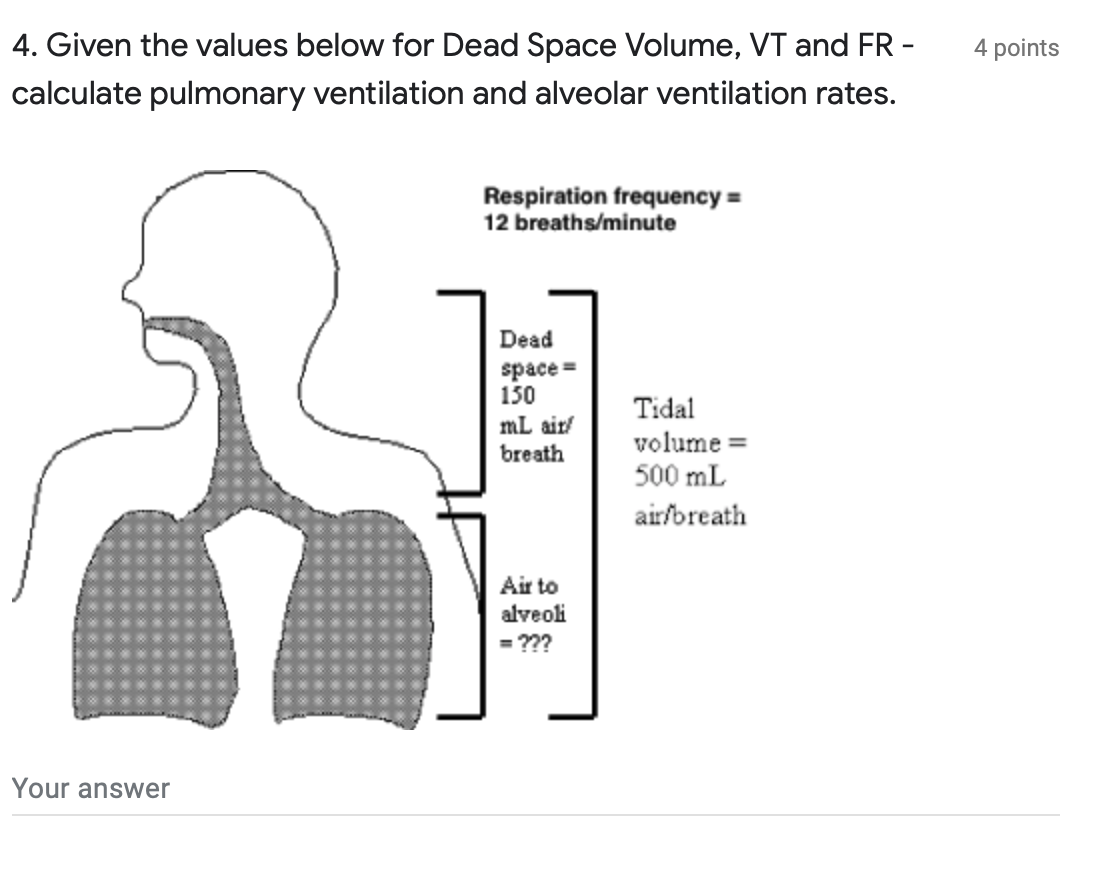
doi: 10.1093/bja/aem166Ĭhoi EM, Na S, Choi SH, An J, Rha KH, Oh YJ. Respiratory and haemodynamic effects of volume-controlled vs pressure-controlled ventilation during laparoscopy: a cross-over study with echocardiographic assessment. doi: 10.1016/j.jmig.2009.10.007īalick-Weber CC, Nicolas P, Hedreville-Montout M, Blanchet P, Stéphan F. Pressure-controlled vs volume-controlled ventilation during laparoscopic gynecologic surgery. Oğurlu M, Küçük M, Bilgin F, Sizlan A, Yanarateş O, Eksert, et al. Lung-protective properties of expiratory flow-initiated pressure-controlled inverse ratio ventilation: A randomised controlled trial. Hirabayashi G, Saito M, Terayama S, Akihisa Y, Maruyama K, Andoh T. Effect of pressure-controlled inverse ratio ventilation on dead space during robot-assisted laparoscopic radical prostatectomy: A randomised crossover study of three different ventilator modes. Hirabayashi G, Ogihara Y, Tsukakoshi S, Daimatsu K, Inoue M, Kurahashi K, et al. Abbreviations: VD phys, physiological dead space VD aw, airway dead space VD alv, alveolar dead space VD shunt, shunt dead space V TE, expired tidal volume VCO 2, expired tidal volume of CO 2 FCO 2, fractional concentration of CO 2 P ECO 2, mixed expired partial pressure of CO 2 P ETCO 2, end-tidal partial pressure of CO 2 P ACO 2, alveolar partial pressure of CO 2 and PaCO 2, arterial partial pressure of CO 2 are expressed as FCO 2 in this figure. Thus, alveolar dead space (VD alv) is calculated as VD resp−VD aw, shunt dead space (VD shunt) is calculated as VD phys−VD resp. The volume from the start of expiration to the partial pressure of mixed expired CO 2 point on the Y axis is defined as respiratory dead space (VD resp). The VD aw is determined by applying Fowler’s equal area method (area A equals to B). Phase II ends at the inner square area maximum point. Phase I represents CO 2-free and pure dead space, phase II represents the transition between airway and alveolar gas, and phase III represents alveolar gas. The expired tidal volume on the Y axis is plotted against the partial pressure of expired CO 2 on the X axis in order to express the curve of ‘Volume = VCO 2/FCO 2’. However, the shunt dead space rate increased with time, suggesting that atelectasis developed with time in both groups. Pressure-controlled inverse ratio ventilation reduced the physiological dead space rate, suggesting an improvement in the total ventilation/perfusion mismatch due to improved inflation of the alveoli affected by heterogeneous expansion disorder without hyperinflation of the normal alveoli. There were no significant changes in the alveolar dead space rate. The airway dead space rate increased with time, but the difference between the groups was not significant. 
The physiological dead space and shunt dead space rate were decreased in the pressure-controlled inverse ratio ventilation group compared with those in the volume control ventilation group (p < 0.001 and p = 0.003, respectively), and both dead space rates increased with time in both groups. The influence of pressure-controlled inverse ratio ventilation and time factor on the changes in each dead space component rate was analyzed using the Mann-Whitney U test and Wilcoxon's signed rank test. Using volumetric capnography, the physiological dead space was divided into three dead space components: airway, alveolar, and shunt dead space. The inspiratory to expiratory ratio was adjusted individually by observing the expiratory flow-time wave in the pressure-controlled inverse ratio ventilation group (n = 14) and was set to 1:2 in the volume-control ventilation group (n = 13). 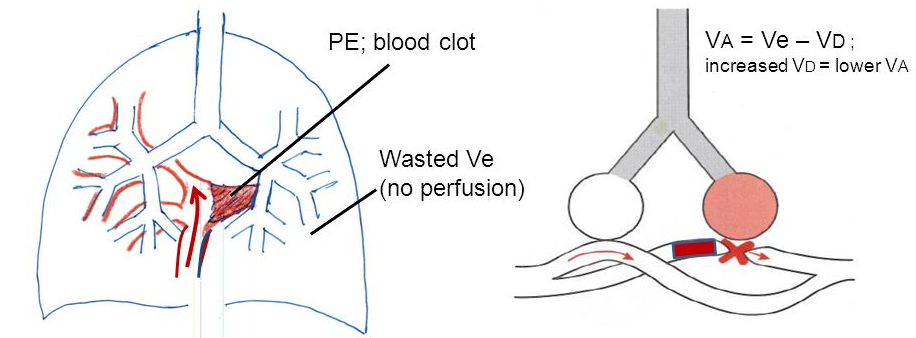
This study was a secondary analysis of a randomized controlled trial of patients who underwent robot-assisted laparoscopic radical prostatectomy. Dead space represents a ventilation-perfusion mismatch, and can enable us to understand the heterogeneity and elapsed time changes in ventilation-perfusion mismatch. We previously reported that there were no differences between the lung-protective actions of pressure-controlled inverse ratio ventilation and volume control ventilation based on the changes in serum cytokine levels.
0 Comments
Leave a Reply. |
Details
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
